|
Back in May I travelled to the Netherlands to be a teaching assistant for the Restorative Exercise™ Specialist (RES) Certification Week. I was fortunate to meet so many amazing people from all over the world! One person that made a big impression on me was David McCoid (pictured here on the left). David certified as a RES back in April 2014 and was in the Netherlands for a few days to soak in the learning.
I got to chat with him on our commute one morning and was so blown away by his personal journey out of pelvic pain. As a pelvic health specialist, his experience really lit up for me: David lived with pelvic pain for 14 years, he travelled to see specialists in Italy for prostate injections, and in the US for pelvic PT treatments with renown therapists, and finally had pudendal nerve surgery (3 different times!). Eventually he found Restorative Exercise™ and he was able to move himself out of pain! I was so inspired by his story that I wanted share his experience. David has asked me to delete his interview because he is not practicing the Katy Bowman method anymore. |
|
Susan McLaughlin is a physical therapist who specializes in the management of pelvic floor and orthopedic dysfunctions. She is the owner of ALIGN integration|movement in Salt Lake City, UT. Helpful tips and other self care strategies can be found at www.alignforhealth.com.
2 Comments
As I mentioned above, the joint is simple, but the function is complex because the hip joint, like any other joint in the body, does not work/move in isolation. Lack of hip range of motion can effect the health of the shoulders, spine, pelvis, knees and feet. Improving hip joint motion is one of the key steps to ensure proper mechanics of the extremities and the spine. How are your hips? Try these moves for better movement.
Susan McLaughlin is a physical therapist who specializes in the management of pelvic floor and orthopedic dysfunctions. She is the owner of ALIGN integration|movement in Salt Lake City, UT. Helpful tips and other self care strategies can be found at www.alignforhealth.com.
 This month I was interviewed by a colleague of mine from the Neurokinetic Therapy™ Community, Eric Nelson. Eric Nelson is a chiropractor and owner of Nelson Chiropractic and Pilates Center. Not many people specialize in pelvic health, so he wanted to pick my brain about pelvic health. He asked me some great questions about pelvic health so I thought that it would be a good idea to share the interview on my blog. Some of the topics discussed:
Inside the Brain Of: Susan McLaughlin, PT Susan McLaughlin is a physical therapist who specializes in the management of pelvic floor and orthopedic dysfunctions. She is the owner of ALIGN integration|movement in Salt Lake City, UT. Helpful tips and other self care strategies can be found at www.alignintegrationandmovement.com.
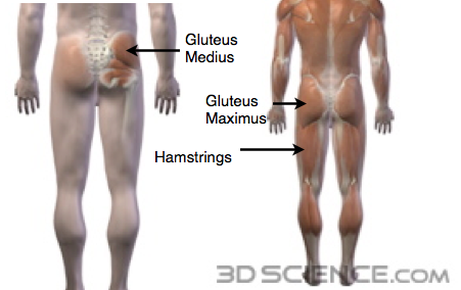 Posterior chain muscles used during the squat. Posterior chain muscles used during the squat. If you didn't know already, the squat is hot. Everybody is doing it..... The squat is one of the most effective ways to strengthen your glutes. But.... not every body is ready to bust the move and go deep into the squat position without losing their balance or hurting their knees. This post demonstrates how to perform a double leg squat and a single leg squat with a vertical shin. A vertical shin helps take the load from the knees and puts the weight back into the posterior chain: hamstrings and glute max. The single leg squat also engages the gluteus medius, which is important for stabilizing the pelvis.
Susan McLaughlin is a physical therapist who specializes in the management of pelvic floor and orthopedic dysfunctions. She is the owner of ALIGN integration|movement in Salt Lake City, UT. Helpful tips and other self care strategies can be found at www.alignintegrationandmovement.com.
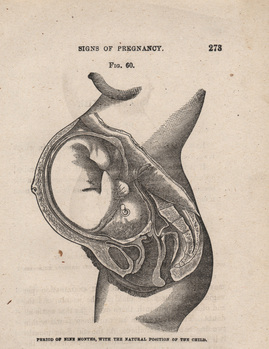 Recently I had a conversation with a doula about fetal positioning. She and many of her doula colleagues have noticed an increase in clients that struggle during labor due to posterior positioning of the fetus. Posterior occiput position is when the baby's head is down and facing mom's belly. A normal presentation is when the head is down and the baby's head is facing the mom's sacrum as in the picture to the left. I would like to share some information from the workshop I presented to our Salt Lake Birth Circle group. Incidence and consequences of Occiput Posterior (OP):
Why are babies malpositioned?Penny Simkin, PT and author of The Labor Progress Handbook attributes fetal malposition to cultural habits and trauma. Cultural Habits:
What can we do about it?
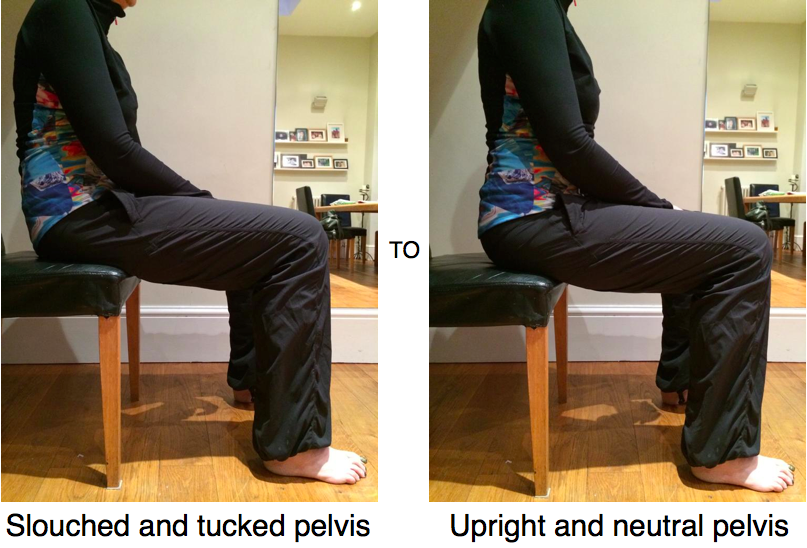
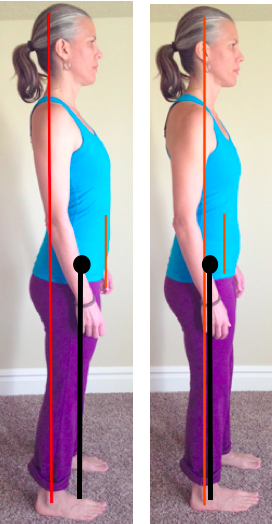
Stand and Sit AlignmentRelease Tension in your Hip Flexors and Pelvic FloorIf you are in the Salt Lake area you can learn about the topics introduced in this blog and more, in my prenatal workshop, Birth Mechanics: Get Your Body Tuned up for Delivery. Susan McLaughlin is a physical therapist who specializes in the management of pelvic floor and orthopedic dysfunctions. She is the owner of ALIGN integration|movement in Salt Lake City, UT. Helpful tips and other self care strategies can be found at www.alignintegrationandmovement.com.
What contributes to bunions and neuromas?
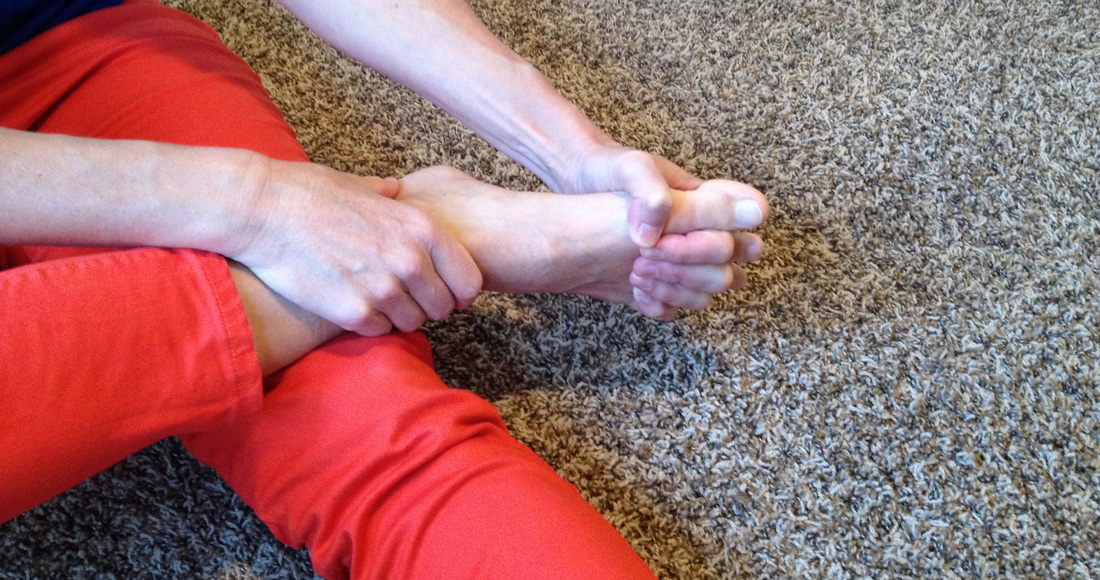
Simple Steps to Eliminate Foot Pain 1. Take a piece of blank paper. Stand barefoot on the paper and outline your foot with a pen. Take this paper to your closet and compare the width of your shoes to the outline. Don't wear the shoes where you can't fit your toes in the toe box, and the outline extends beyond the shoe. Notice that the shoe sits inside of the outline in some places; don't wear these shoes! Find shoes that do not have a heel. If you are used to wearing a higher heel you will need to gradually transition to lower heels so your tissues have time to adapt (give yourself 4-6 wks before you transition for each .5 to 1 inch). 2. Learn how to stand in alignment. See pic above. Or read this blog. 3. Wear toe spacers. Yes, you should be able to see space between your toes! There are many products on the market. These are my favorite: Correct Toes. Cool thing about these is that you can wear them in your shoes! Very comfortable (but you have to have a wide enough toe box in your shoe). If you have a bunion you may want to test to see if this will be comfortable for you before purchase: take your big toe and pull it away from your other toes as far as you can, and then lift it up. If there is discomfort in the joint then your toe is probably compressed, and it would be good for you to see me, or your local PT (or chiro, osteo, etc) to work with you. Exercise your feetSusan McLaughlin is a physical therapist who specializes in the management of pelvic floor and orthopedic dysfunctions. She is the owner of ALIGN integration|movement in Salt Lake City, UT. Helpful tips and other self care strategies can be found at www.alignintegrationandmovement.com.
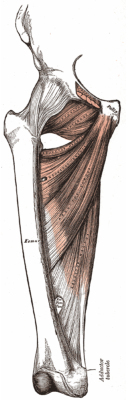 The inner thigh (adductor group) is made up of five muscles:
When the foot is not planted on the ground, the adductors will bring the leg toward the midline, and flex the hip when the thigh is in an extended position as in the swing phase of the gait (walking) cycle. The adductors play a significant role during walking and are active in all phases of the gait cycle. The adductors are a part of two important functional kinetic chains:
Dysfunction within the slings can result in overuse of the adductor group leading to over facilitation, increased tension and bound up connective tissue, and potentially pain. Here is a videoblog demonstrating how to release the adductors using a foam roller. Susan McLaughlin is a physical therapist who specializes in the management of pelvic floor and orthopedic dysfunctions. She is the owner of ALIGN integration|movement in Salt Lake City, UT. Helpful tips and other self care strategies can be found at www.alignintegrationandmovement.com.
 Tension in the piriformis muscle can trigger irritation of surrounding tissues. The sciatic nerve exits the pelvis just below the piriformis. When there is dysfunction in the lumbo/pelvic/hip complex, the piriformis often gets overworked, creating compression and friction on the sciatic nerve. Sciatica is defined as aching/burning/stinging pain along the distribution of the sciatic nerve: buttock, back of the thigh, lower leg and foot. Stretching the piriformis can be a very effective way of diminishing the compression, and therefore irritation of the nerve. Pictured to the left is a very common stretch given as treatment to relieve sciatica. Piriformis Stretch RefinedA traditional piriformis stretch, is often done with a tucked pelvis (and/or flexed spine) and can irritate the nerve if the leg is pulled too aggressively. Instead, using the wall and props can be an effective way of maintaining a neutral spine and pelvis. By staying in alignment, and by being able to adjust the load by gradually bending the knee to 90 degrees, the tissues will begin to yield and let go, rather than work to hold the body in position. Picture on the left: The half cylinder and block supports my shoulders and head to allow me to rest with a neutral spine, with my ribs down and a level pelvis. Due to my current tension patterns, I also have to support my lumbar area with a rolled yoga mat so I can comfortably attain neutral pelvis (pubis and ASIS level). Middle picture: I place my left leg straight on the wall and cross my right leg over the left, making sure not to tilt the pelvis. Picture on the right: I begin to slide my heel down the wall and stop when I feel that I am at my resistance barrier, or my pelvis begins to shift. Hold at least one minute and repeat on the other side. If you can tolerate the stretch stay longer, up to 5 minutes on each side. Some people will try to get a deeper stretch by pressing the right knee down. Make sure that you don't drag your whole pelvis when you do that (as shown in the pic on the left). The purpose of this refinement is to maintain neutral, and that means a level pelvis (as shown on the right). Even if you don't have sciatica, this is a wonderful stretch to open the hips, and allow more freedom to your pelvis! Enjoy! Susan McLaughlin is a physical therapist who specializes in the management of pelvic floor and orthopedic dysfunctions. She is the owner of ALIGN integration|movement in Salt Lake City, UT. Helpful tips and other self care strategies can be found at www.alignintegrationandmovement.com.
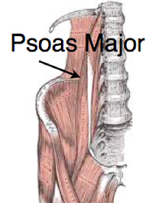
 The dot and arrow show pelvic posterior rotation. The dot and arrow show pelvic posterior rotation. Legs on the wall pose is a restorative position that should be a staple for every person that has a pelvis! Traditionally, the pose is taught by placing the butt close to the wall, and then bringing the legs up against the wall so the back of the legs touch, and the soles of the feet are facing the ceiling. A variation to the pose is to widen the legs into a "V" position to stretch the inner thighs and groin. Recently I have rediscovered the beauty of this pose by modifying the position to be able to maintain neutral pelvis (pubis and ASIS in line) and rib alignment. The benefit of maintaining the alignment markers during this pose allows the connective tissue and muscles to fully release. When the alignment markers are not in place, there is more load to the tissues which can potentially maintain tension, and prevent a full yield ("letting go") of the muscles and fascia. In order to do this pose in alignment, you may need to get out props. Due to the tightness of my psoas muscles and the increased kyphosis of my thoracic spine, I have used a thin yoga mat rolled up to maintain neutral pelvis: pubis and ASIS level, and a half cylinder & block to prop up my upper back to get my lower ribs down and flush with my abdomen. In order to get my pelvis level, I needed to scoot away from the wall, get the props set up, and then place my legs on the wall (see pics below). Benefits to Legs on the Wall Pose:
Legs on the Wall Pose in AlignmentSusan McLaughlin is a physical therapist who specializes in the management of pelvic floor and orthopedic dysfunctions. She is the owner of ALIGN integration|movement in Salt Lake City, UT. Helpful tips and other self care strategies can be found at www.alignintegrationandmovement.com.
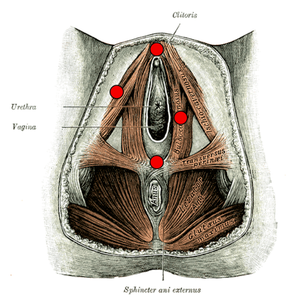
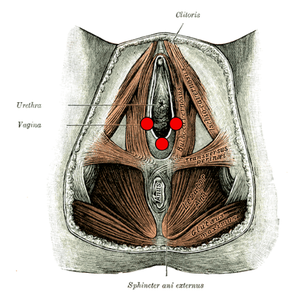
Do you experience burning, stinging or rawness in your vulvar area? Maybe you feel itching, throbbing, or aching in the perineum and pelvis. You are not alone. These symptoms are typical of vulvodynia. Vulvodynia is a pain condition of the female genitals: clitoris, vestibule (vaginal opening), labia, and perineum. There are two main subtypes of vulvodynia:
Self Care StrategiesSelf-care and treatments for vulvodynia can help bring relief and recovery. Unfortunately, there is not a "one size fits all" treatment. Working with a trained healthcare provider who understands vulvodynia is crucial to getting out of pain. Here are a few suggestions to alleviate symptoms: Avoid Irritants to the vulvar tissue
Relieve pain and ease pressure
Make an appointment with your local Pelvic Health Physical Therapist
Resources Susan McLaughlin is a physical therapist who specializes in the management of pelvic floor and orthopedic dysfunctions. She is the owner of ALIGN integration|movement in Salt Lake City, UT. Helpful tips and other self care strategies can be found at www.alignintegrationandmovement.com.
|
AuthorSusan McLaughlin, FEEL GOOD SERIES:
|
|
|
Archives
November 2022
May 2022
November 2021
April 2021
December 2020
September 2020
July 2020
June 2020
May 2020
April 2020
February 2020
October 2019
September 2019
August 2019
July 2019
March 2019
January 2019
December 2018
November 2018
September 2018
August 2018
June 2018
March 2018
February 2018
January 2018
December 2017
November 2017
October 2017
August 2017
July 2017
May 2017
March 2017
February 2017
January 2017
December 2016
November 2016
September 2016
August 2016
July 2016
June 2016
May 2016
April 2016
February 2016
January 2016
December 2015
November 2015
October 2015
September 2015
August 2015
July 2015
June 2015
May 2015
February 2015
January 2015
December 2014
November 2014
October 2014
August 2014
June 2014
May 2014
March 2014
February 2014
January 2014
December 2013
November 2013
October 2013
August 2013
July 2013
June 2013
May 2013
March 2013
January 2013
December 2012
November 2012
October 2012
September 2012
August 2012
July 2012
June 2012
May 2012
April 2012
March 2012
February 2012
January 2012



























 RSS Feed
RSS Feed